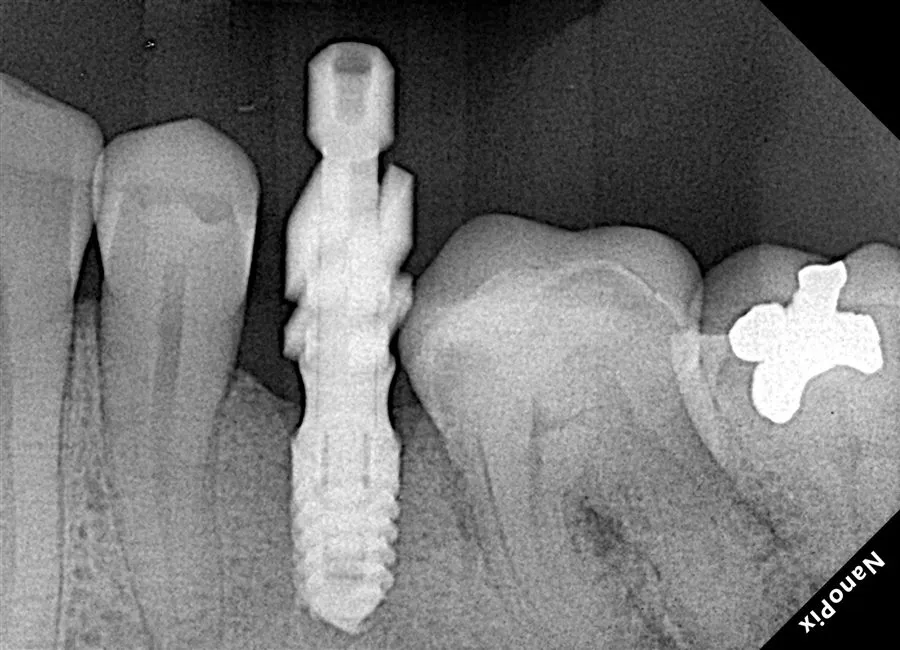
The Short Answer
A suitable dental implant candidate is usually someone with one or more missing teeth, enough healthy jawbone to hold the implant, stable gum health, manageable medical risk factors and realistic expectations about surgery, healing and maintenance.
That does not mean you need a perfect mouth before an implant can be discussed. Some people need gum treatment, tooth removal, bone grafting, sinus lift treatment or changes to the planned restoration before implant placement is appropriate. The key is careful assessment before surgery, not assuming every missing tooth should be treated in the same way.
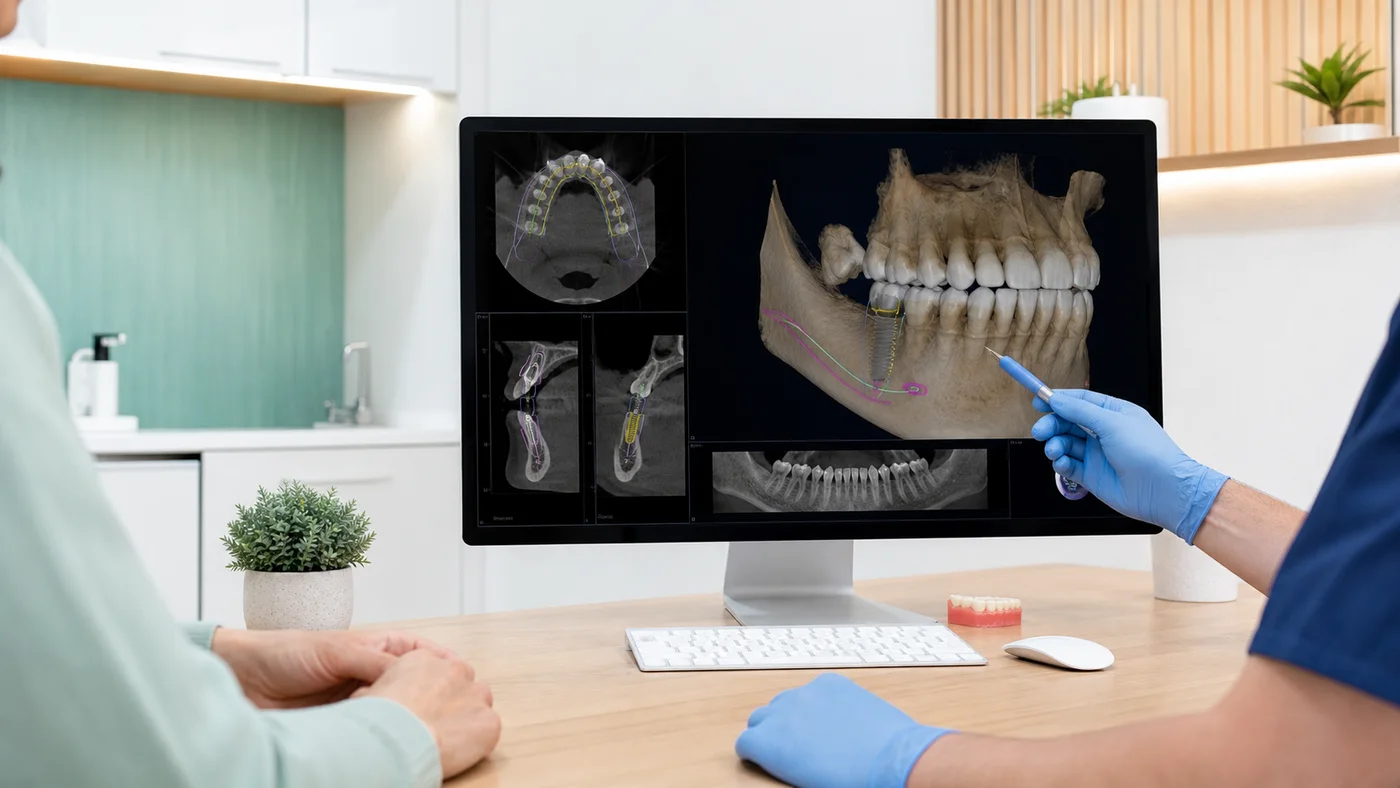
Suitability is individual
This article is general information. A dental implant decision needs a clinical examination, imaging and a discussion of alternatives, risks, costs and maintenance.
What Makes Someone More Suitable?
The main question is whether an implant can be placed in a position that supports a functional, cleanable and maintainable crown, bridge or denture. Your dentist will usually consider the following areas.
| Factor | Why it matters | What may be checked |
|---|---|---|
| Jawbone volume | The implant needs adequate bone height and width for stable placement and long-term support. | CBCT scan, ridge shape, sinus position, nerve location and whether grafting is needed. |
| Gum health | Active gum disease can increase infection risk and may affect the bone around teeth and implants. | Periodontal charting, bleeding, pocket depths, cleaning access and oral hygiene habits. |
| General health | Healing and infection risk can be affected by medical conditions, immune status and medications. | Diabetes control, osteoporosis medicines, blood thinners, immune suppression and medical history. |
| Smoking and vaping | Smoking is associated with delayed healing and higher implant complication risk. | Smoking history, readiness to stop or reduce, and timing around surgery. |
| Bite forces | Grinding, clenching or heavy bite forces can overload the implant restoration. | Tooth wear, jaw symptoms, bite pattern, restoration design and night guard suitability. |
| Maintenance ability | Implants need daily cleaning and professional review because surrounding gum and bone can become inflamed. | Cleaning tools, access around the restoration, recall schedule and long-term hygiene plan. |
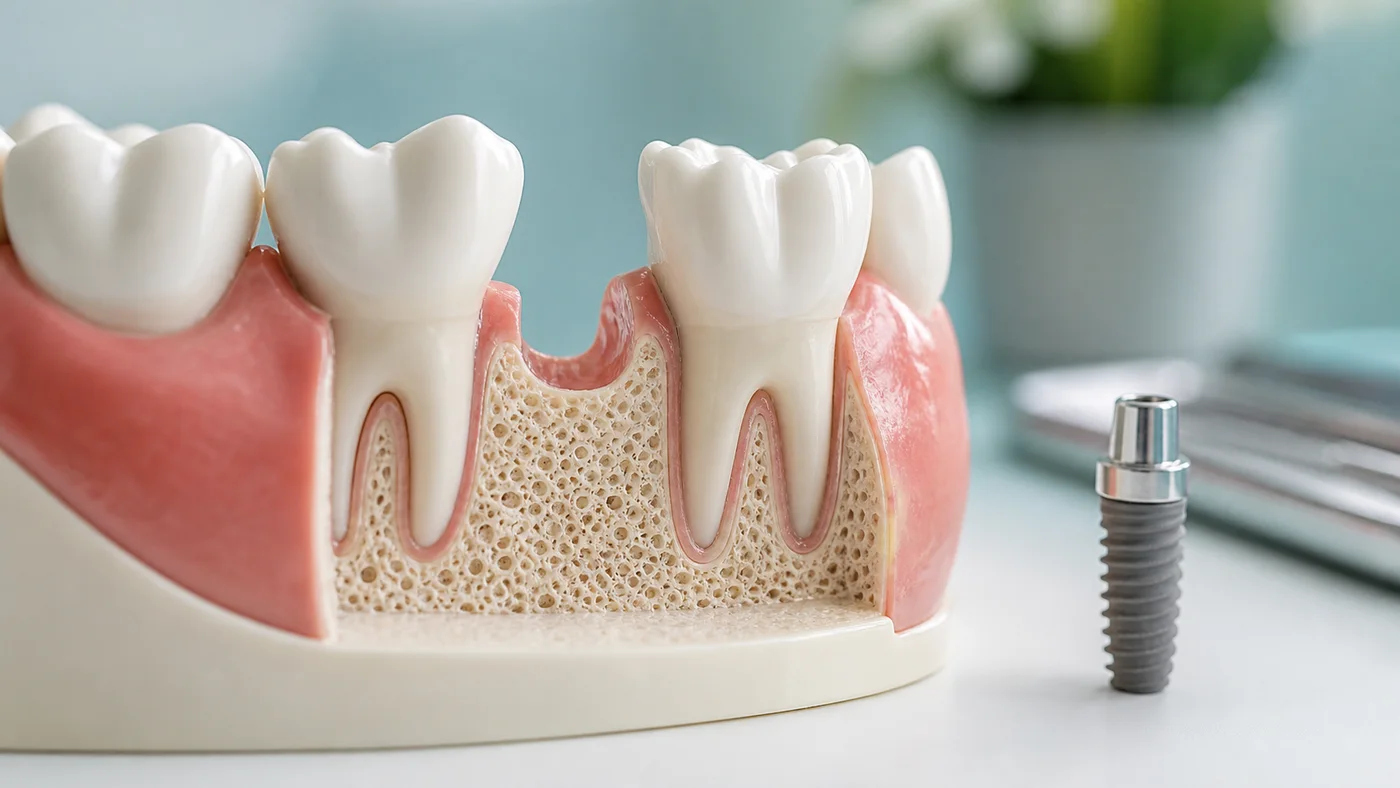
When Might an Implant Need to Wait?
An implant may need to be delayed or reconsidered when risk factors are active or uncontrolled. This is not always a permanent "no"; often it means the mouth or general health needs to be stabilised first.
Active gum disease
Periodontal treatment may be needed before implant placement is planned, especially if there is bleeding, pocketing or ongoing bone loss.
Inadequate bone
Bone loss after tooth loss, infection or trauma can mean grafting, sinus lift treatment or a different restoration design is needed.
Uncontrolled medical risks
Diabetes control, immune suppression, certain medications and bleeding risk may need medical coordination before surgery.
Heavy smoking
Smoking can affect healing and implant integration. Your dentist may recommend stopping before and after surgery to reduce risk.
There are also situations where an alternative to implants may be more appropriate. Options can include a removable denture, resin-bonded bridge, conventional bridge, staged tooth treatment or no immediate replacement, depending on the case.
What if There Is Not Enough Bone?
Tooth loss often leads to changes in jawbone shape. If the bone is too narrow, too short or too close to the sinus or nerve, implant treatment may need extra planning.
For some patients, bone grafting, ridge preservation or a sinus floor elevation may help create better support for a future implant. In other cases, the dentist may recommend a different implant position, a bridge design, full-arch planning or a non-implant option.

Earlier assessment can help
If a tooth is failing or has recently been removed, an implant assessment can help decide whether socket preservation or staged grafting should be discussed before the bone changes further.
How Suitability Is Checked
A suitability assessment usually combines what you want from treatment with what the anatomy and health of the mouth can support. At Brisbane Dental Implants, this may include discussion of your goals, dental examination, gum assessment, bite review and 3D CBCT imaging where indicated.
The final plan should explain the proposed implant option, alternatives, likely timeframes, costs, risks and maintenance. For example, a single tooth implant is planned differently from All-on-4 or full mouth dental implant treatment.
Questions worth asking
- Do I have enough bone for the implant position being proposed?
- Is there any gum disease or infection that needs treatment first?
- Do my medical history or medications change the risks?
- Do I need grafting, a sinus lift, temporary teeth or staged treatment?
- How will I clean the implant restoration at home?
- What are my realistic alternatives if I choose not to have an implant?
Common Questions
A suitable candidate usually has enough jawbone, stable gum health, manageable medical risk factors, realistic expectations and a bite that can support the planned restoration. A dental professional needs to confirm this with examination and imaging.
Active gum disease may need to be treated before implant placement is considered. Stable gums and a long-term maintenance plan are important because inflammation can affect the bone around implants.
Sometimes. Bone grafting, sinus lift treatment or a different restoration design may be discussed depending on the amount and location of bone loss.
Smoking is associated with delayed healing and increased implant complication risk. Your dentist may recommend stopping before and after implant surgery.
Sources Used
This article was informed by Australian dental and health guidance. It is general information only and does not replace an individual clinical assessment.
Wondering if implants may suit you?
Book a clinical assessment to discuss your bone, gum health, treatment options and written quote.