Socket preservation
Graft material is placed at the time of extraction to reduce ridge collapse and preserve the site for later implant placement. It may be recommended when immediate implant placement is not suitable.
Bone grafting can rebuild or preserve jawbone so a dental implant has enough support. This guide explains socket preservation, ridge augmentation, sinus lift, costs, healing times, risks and when grafting may not be needed.
Bone and Implant Assessment
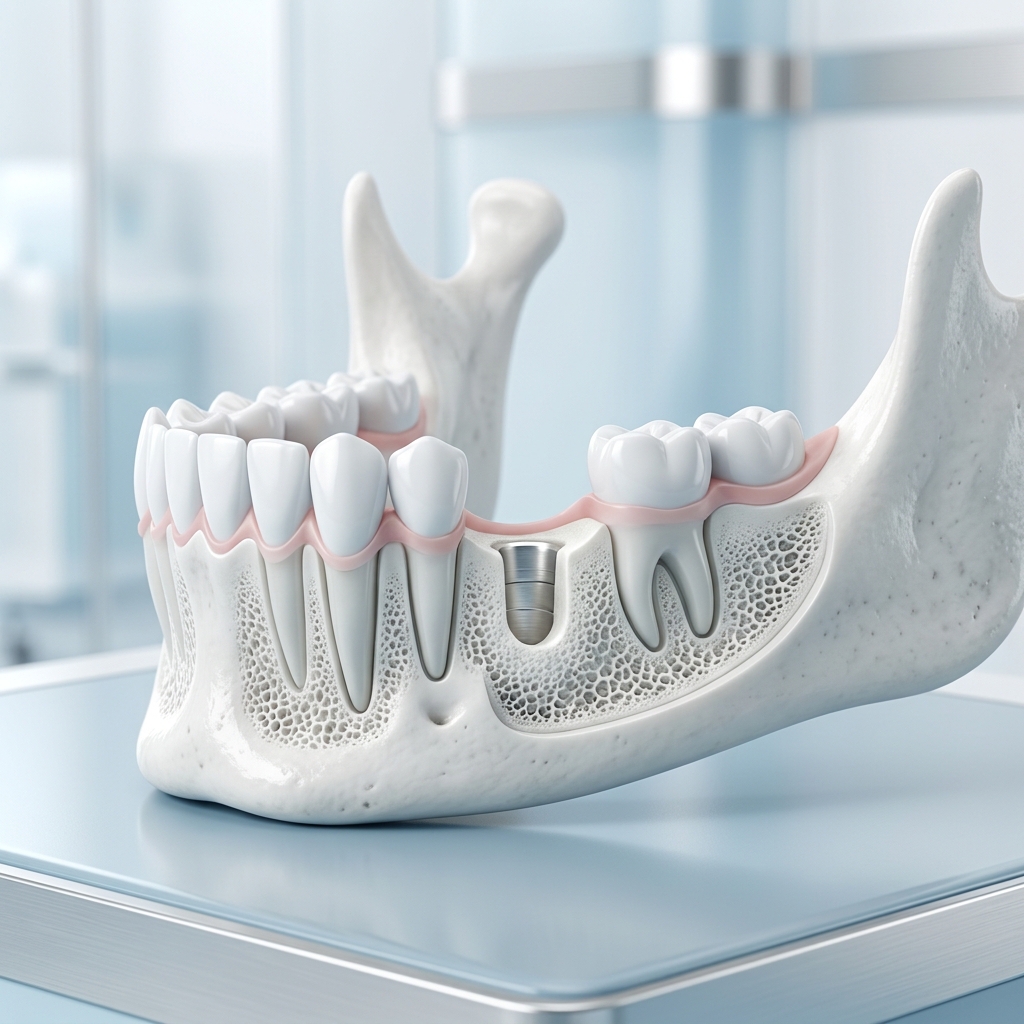
A dental implant needs enough bone to hold the fixture in a stable position and support the final crown, bridge or denture. After a tooth is removed, the socket changes shape as it heals. Bone can shrink in height and width, especially where infection, trauma or gum disease has damaged the area.
Bone grafting uses graft material to preserve or rebuild the implant site. The goal is not simply to add bulk. The goal is to create bone volume in the right position so the implant can be placed in a functional, cleansable and restorative position.
Grafting is not always required. Some sites already have enough bone, and some full arch plans use angled implants to work with available anatomy. In other cases, grafting may reduce compromises in implant angle, crown shape, hygiene access or long-term support.
The type of graft depends on the defect shape, tooth position, sinus location, infection history and implant plan.
Your clinician should explain the graft material, why it is recommended and whether alternatives exist.
Healing time depends on graft size, location, infection history, material used and whether implant placement is simultaneous or delayed.
The dentist assesses bone volume, defect shape, nerve and sinus location, gum thickness and the future implant position.
Active infection, gum disease or failing teeth may need management before or during grafting so the site can heal more favourably.
Graft material is placed in the planned area and may be covered with a membrane. Sutures protect the site while early healing begins.
Minor socket grafts may heal in a few months. Larger ridge grafts or sinus lifts can require longer before implant placement is considered.
Once the graft has matured sufficiently, implant placement is planned. Sometimes the implant and graft can be placed at the same appointment.
Bone grafting fees vary because a small socket preservation graft is very different from a larger ridge augmentation or sinus lift.
Socket preservation at extraction is often a smaller procedure. Fees depend on the tooth, defect, graft material and whether other treatment is performed at the same visit.
Ridge augmentation, sinus lift and staged grafting can involve more materials, imaging, surgical time and follow-up. These are quoted after examination and CBCT review.
Grafting can add cost, but it may support a better implant position. Compare this with the dental implants cost Brisbane guide.
Bone grafting has risks like any surgical procedure. Your treating practitioner should explain the risks relevant to your anatomy and health.
The examples below show treatment categories where bone support can influence implant planning. They are not predictions of outcome.
Bone grafting at Brisbane Dental Implants is assessed by the treating dentist using clinical examination and 3D imaging. Dr Virginia Han and Dr Sae Mi Bok have a clinical focus on implant site planning, bone support and restorative outcomes, with treatment recommendations made after individual assessment.
Return to dental implants hubGood aftercare protects the graft while early blood supply and tissue closure develop. Your instructions may vary depending on the size and location of the graft.
Call the clinic if you notice increasing swelling after the first few days, persistent bleeding, unpleasant taste, fever, wound opening, graft particles coming out in large amounts, numbness, sinus symptoms or pain that is worsening rather than settling. Some minor granules may appear after certain grafts, but your team can tell you what is expected for your procedure.
After the graft matures, the implant plan may be confirmed with further imaging or clinical review. The dentist checks whether the graft has created enough bone in the right position. If the result is not adequate, the plan may be adjusted before implant placement.
Bone grafting decisions depend on the defect, the implant goal and the health of the surrounding tissues.
Bring any recent x-rays, details of when the tooth was removed, history of swelling or infection, periodontal treatment records and information about smoking or vaping. If you have had previous grafting, sinus surgery, implant failure or difficult extractions, tell the clinician before treatment planning begins.
Ask what type of defect is present: is the bone too narrow, too short, affected by the sinus, affected by infection, or missing on the cheek side of the socket? The answer should connect directly to the recommended graft type and the future implant position.
Useful questions include what graft material is proposed, whether a membrane is needed, whether implant placement can happen at the same time, how long healing is expected to take, what aftercare is required and what the backup plan is if the graft does not provide enough bone for the original implant plan.
No. Some implant sites have enough bone. Grafting is considered when bone height, width or position may compromise implant placement or the final restoration.
Sometimes. Simultaneous grafting and implant placement depends on primary stability, defect size, infection status and the planned restoration.
Minor grafts may be ready in a few months. Larger grafts or sinus lifts can take longer. The timing is confirmed by clinical healing and imaging.
The plan may need modification, additional grafting or a different restoration. Your dentist should discuss this possibility during consent.
It can be helpful when an implant is likely later and immediate placement is not suitable. It aims to reduce bone shrinkage after extraction.
Read the main implant hub, single tooth implant guide, All-on-4 guide and cost guide.
Book a free implant consultation at Brisbane Dental Implants to discuss your treatment options with a plan tailored to your mouth.
Submit your details to arrange a clinical assessment.